No products in the cart.
blog
Rosette-Shaped Cataract
A 56-year-old male patient went to an outpatient department (OPD) with complaints of diminution of vision in the left eye for the last 1 year. He gave no history of any glare or difficulty at night. He did not have any relevant past history of any trauma (blunt or subtle, even after repeated questioning) nor of any ocular or systemic disease. He gave no significant personal history, was not a smoker, or gave no drug addiction history. He was a spectacle wearer using a bifocal with distance correction +1.00 Dioptre Sphere (DS) in both eyes and a near correction of +2.50DS in both eyes. His best-corrected visual acuity (BCVA) was right eye (oculus dexter) (OD) 6/6, N6, and left eye (oculus sinister) (OS) 6/18, N6. On examination, he was found to have a “double rosette cataract” in the left eye, with early lens changes in the right eye. Gonioscopy, indirect ophthalmoscopy, and ultrasound biomicroscopy (UBM) were carried out to rule out any signs of subtle trauma and revealed no significant abnormality. The remaining examination did not reveal any significant findings. Furthermore, on examining his sibling and children no signs of any developmental cataract or similar lens abnormalities were noted. Suggesting that there was no significant family history suggestive of a similar “double rosette cataract,” thereby ruling out any familial or hereditary traits.
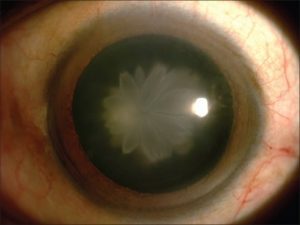
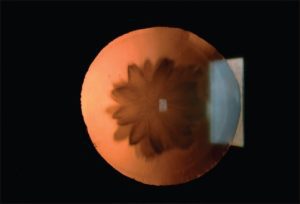
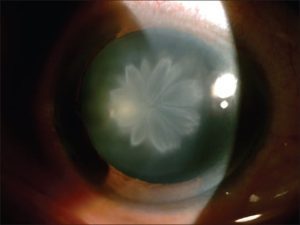
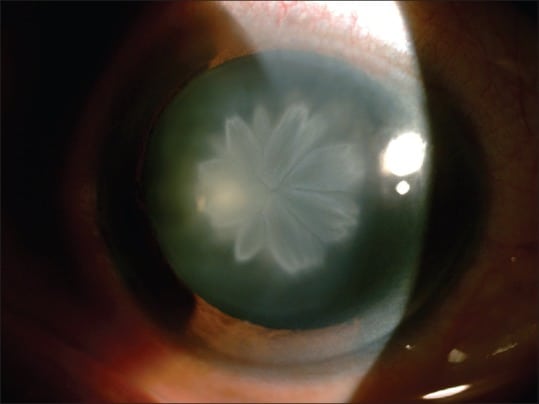
Another case of Rosette Cataract on slit-lamp [3]
Discussion
Rosette or stellate-shaped cataracts are associated with blunt injury of the eye.[1] the patient gave no such history of any trauma, any systemic illness, metabolic disease, drug use, or any other significant history leading to this type of cataract. Rosette cataracts are also associated with diabetes mellitus.[2]
Conclusion
Double rosette type of cataract with no history of any trauma or systemic illness has never been reported in the literature before. This is a case of a double rosette cataract found incidentally.
References
1. Fyodorov SN, Egorova EV, Zubareva LN. 1004 cases of traumatic cataract surgery with implantation of an intraocular lens. J Am Intraocular Implant Soc. 1981;7:147–53. [PubMed] [Google Scholar]
2. Ramkumar H, Basti S. Reversal of bilateral rosette cataracts with glycemic control. ScientificWorldJournal. 2008;8:1150–1. [PMC free article] [PubMed] [Google Scholar]
3. Sharjeel Eye youtube channel, https://www.youtube.com/watch?v=unH2c5b_DYQ

Good presentation
thanks for your comment
I like this
It was interesting
thanks for your comment
Impressive, thank you
thanks for your comment
Nice presentation
thanks for your comment